You’re at your newborn’s first checkup and the doctor tells you they couldn’t feel one (or both) of your son’s testes in the scrotum. Or maybe you noticed it yourself during a bath. Either way, you’ve probably gone home with a head full of questions and a heart full of worry.
This guide is written to give you clear, honest answers — the same ones I give parents in my clinic every day.
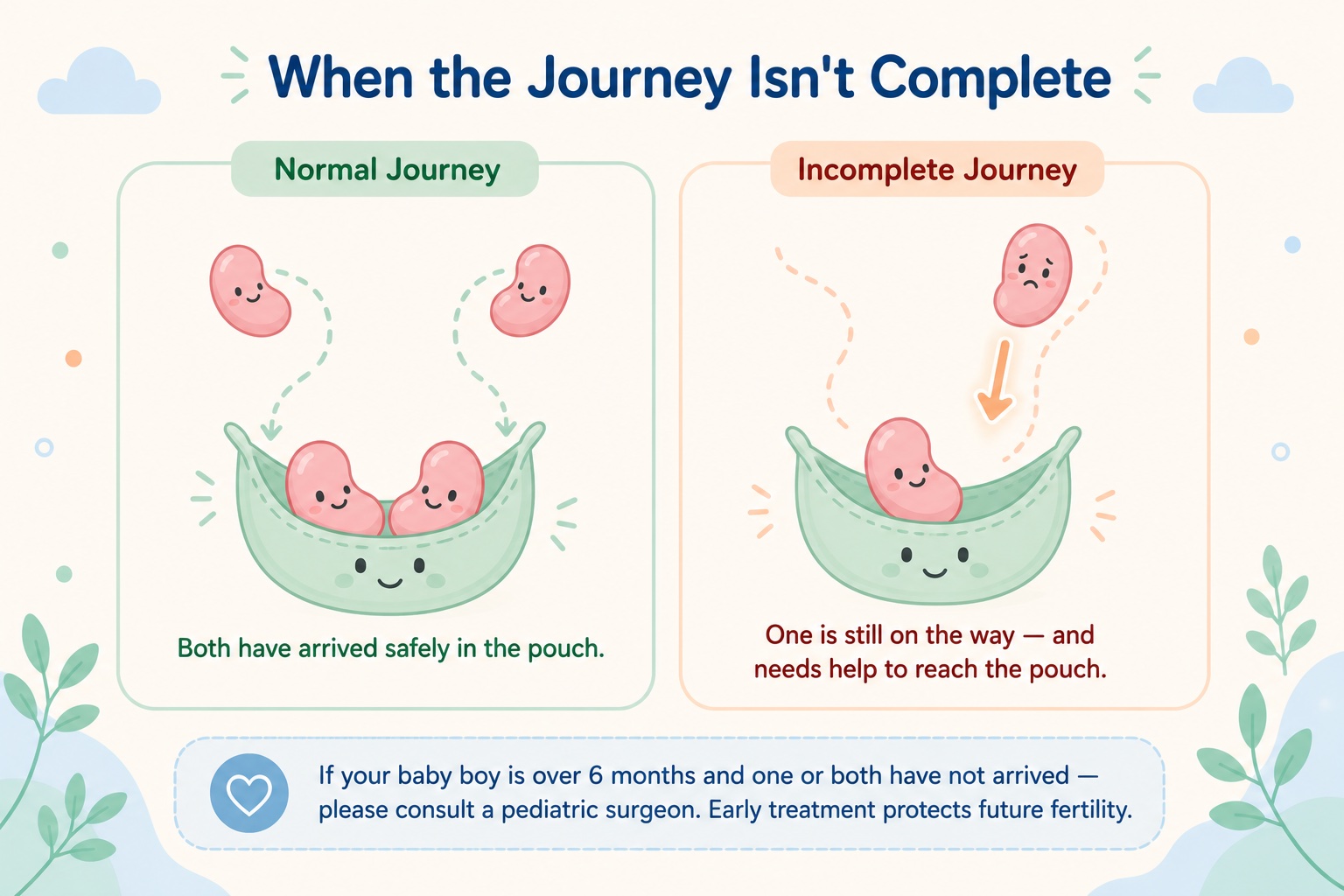
What does “undescended testis” mean?
During pregnancy, the testes form inside the baby’s abdomen and normally descend into the scrotum before birth. In some boys — about 3–5% of full-term babies and up to 30% of premature babies — one or both testes don’t complete this journey. This is called cryptorchidism or undescended testis.
The good news: in about half of cases, the testis descends on its own within the first 3–6 months of life. After 6 months, spontaneous descent becomes very unlikely.
Why does it matter if it’s not treated?
This is where many parents underestimate the issue. An undescended testis is not just a cosmetic concern. If left untreated beyond the recommended age:
- Fertility may be affected — the testis needs the cooler temperature of the scrotum to produce healthy sperm
- Risk of testicular torsion increases — the testis can twist and lose its blood supply (surgical emergency)
- Higher risk of testicular cancer in adulthood — though the absolute risk remains low, it is 3–5x higher than in descended testes
- Psychological impact on the growing child
What is the right age for surgery?
Current international guidelines recommend surgery between 6–18 months of age — ideally by 12 months.
This timing is critical because:
- Earlier surgery preserves more testicular tissue and function
- The window for protecting future fertility is time-sensitive
- Anaesthesia and surgery are safe at this age when performed by a trained team
Do not wait until school age or adolescence. This is a common mistake due to lack of awareness, and it has real consequences.
What does the surgery involve?
The procedure is called orchidopexy — moving the testis from wherever it is (groin, abdomen) down into the scrotum and fixing it there.
- It’s done under general anaesthesia
- Takes 30–60 minutes
- Usually a day-care procedure (home the same day)
- Laparoscopic (keyhole) approach is used for testes that cannot be felt (impalpable testes)
- Recovery is quick — most children are back to normal activity within a week
What if the testis can’t be felt at all?
If you or your doctor can’t feel the testis on examination, it may be:
- In the abdomen (intra-abdominal)
- Absent (vanishing testis — the testis existed but was lost due to blood supply issues during development)
A diagnostic laparoscopy (keyhole camera procedure) is the gold standard for finding an intra-abdominal testis — imaging (ultrasound) is often unreliable in these cases.
Questions parents often ask
“Can we just monitor and wait?”
Only if the child is under 6 months. After that, observation without action is not recommended.
“Is one testis enough? Will my son be fertile?”
One healthy, descended testis is generally sufficient for normal hormone production and fertility.
“Will the surgery affect my son long-term?”
Done at the right age, by a pediatric surgeon, orchidopexy has excellent outcomes. The risk of not treating is far greater than the risk of surgery.
Concerned about your son’s testis? Dr. Tanmay Motiwala is a pediatric surgeon and urologist trained at AIIMS, seeing patients in Raipur, Jagdalpur, and Rajnandgaon. Early assessment saves future complications. Book: +91 8319084711.
⚠️ Important Disclaimer: This article is provided purely for educational and awareness purposes. The information here is not a substitute for medical advice, diagnosis, or treatment, and should not be considered as an OPD or clinical consultation. Every child is different — symptoms that look the same may have different causes. If your child has any of the conditions or symptoms discussed, please consult your nearest qualified pediatric surgeon in person for an examination and personalised advice. In an emergency, go to the nearest hospital immediately.